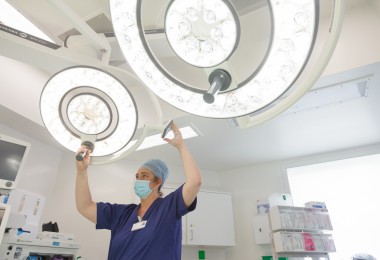
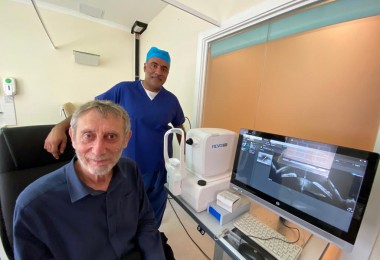
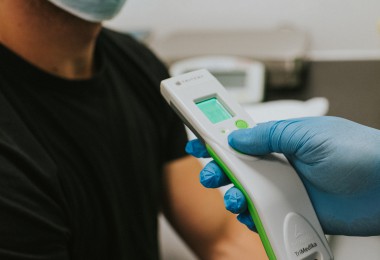
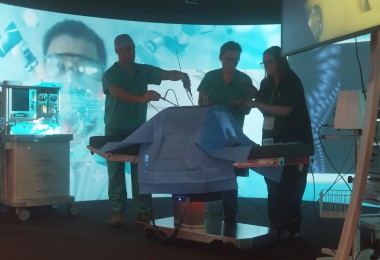
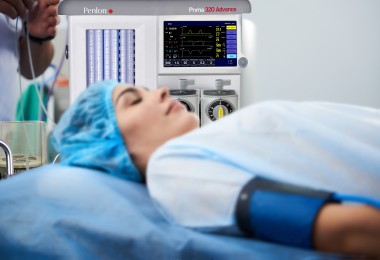
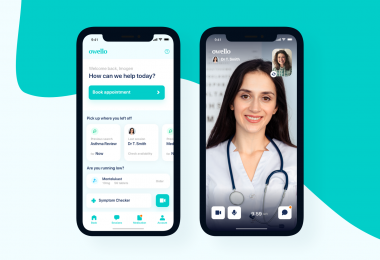
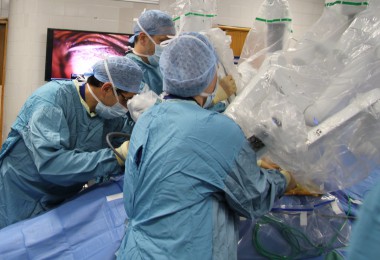
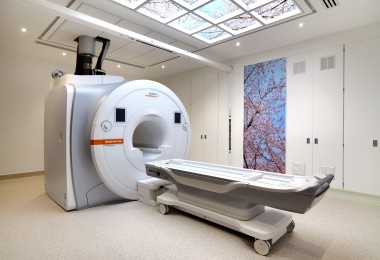
Accurate and timely diagnosis is an essential component of health care, providing vital information to help prevent, treat, and manage disease. Advances in science and technology mean that diagnostic capabilities have evolved to become even more integral to medicine: MRI is now fundamental to interventional radiology procedures, AI-enabled decision support systems are assisting primary care physicians risk assess their patients for cancer more easily, and as the time and costs of conducting whole genome sequencing lower the opportunity to routinely perform genetic diagnosis is realisable.
Capability improvements mean that diagnosis can happen earlier in the care pathway resulting in better treatment outcomes. When cancer is detected at the earliest stages, treatment is more effective and survival drastically improves. Early identification of sepsis followed by rapid initiation of antimicrobial treatment significantly reduces mortality risk.
ABHI’s activity is centred on a vision to make high quality diagnostic technologies accessible to all who need them when they are needed, so that diseases/health conditions can be detected and treated earlier. The NHS spends more than £6 billion a year on over 100 diagnostics services and carries out an estimated 1.5 billion diagnostic tests. Making best use of these resources means identifying at risk populations quickly and accurately, and optimising service requirements to directing individuals to the right treatments.
Several strategic and clinical reviews underscore this shift to earlier diagnosis and the need for radical investment and reform of diagnostic services was recognised at the time the NHS Long Term Plan was published in 2019. NHS England/Improvement have now embarked on a transformation programme to raise capacity, modernise infrastructure and invest in new service models as envisaged in Sir Mike Richards’ report.
System leadership is vital to integrate and align diagnostic modalities not just within hospitals but also between primary and secondary care. The development of integrated care systems should, in the medium/long-term, help complement national coordination with regional implementation.
As new delivery models pull diagnostic services out of hospitals and into the community then data sharing will need to come to the fore. Access to analytics and virtual working means that interoperability between systems is crucial to smooth data flows and technology utilisation across patient journey settings. New requirements announced recently by NHS England to enable this will make a difference.
NICE’s stated intent to increase the use of different types of evidence, with an emphasis on real world evidence sources, will be particularly important for the development of guidance for diagnostics. As should the move to Early Value Assessment for Medtech which will offer a rapid assessment of digital products, devices, and diagnostics for clinical effectiveness and value for money to inform NHS commissioners.
As diagnosis capabilities continue to evolve rapidly through development of new technologies, then that development process will need to adapt to the new regulatory frameworks that are being established for medical devices and diagnostics. The new UK regulatory framework for medical devices and in vitro diagnostic medical devices should act as enablers of new technology allowing patients and clinicians access to innovative diagnostics technologies that meet high unmet clinical need as early as possible through the use of innovative regulatory mechanisms such as target product profiles, common specifications, MHRA premarket role and post market clinical evidence drawn from real world clinical experience and enhanced surveillance methodologies.